Cartilage Repair in Traditional Orthopedics
When it comes to cartilage injury in the knee, medical technology has offered several different surgeries and procedures for its repair.
MACI stands for Matrix-Induced Autologous Chondrocyte Implantation surgery and is popular knee surgery. OATS is an acronym for Osteochondral Autologous Transplantation Surgery. Both of these procedures are attempts to fix holes in the knee’s damaged cartilage.
MACI is a cartilage graft grown from a sample of the patient’s own cartilage. The graft is then glued into the defect or “hole” in the cartilage.
OATS is where a plug of cartilage is taken out of a healthy portion of the bone and implanted into the damaged cartilage defect, or hole.
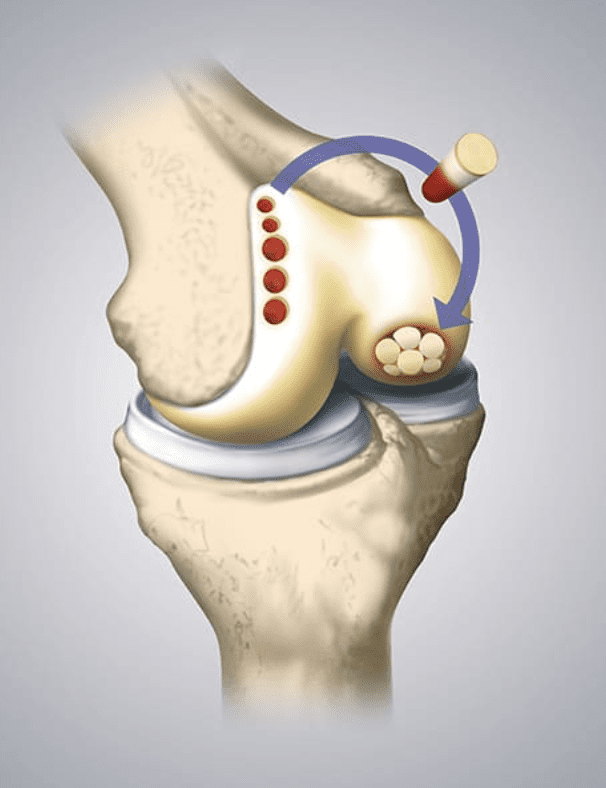
Both of these surgeries, though, are more sophisticated derivatives from an older procedure called microfracture. Microfracture is where the area around the cartilage defect is penetrated to form several tiny holes deep to the level of the bone marrow. The thought is the marrow then becomes available to travel to the injured cartilage tissue and support healing.
The Regenerative Medicine Alternative
Regarding MACI, OATS, and microfracture surgeries, Chris Centeno, MD of the Centeno-Shultz Clinic states:
I’ve seen countless patients through the years who have had each of these surgeries and I’ve never seen one produce a perfect cartilage repair. Microfracture often leaves dead bone behind or large bone spurs in the cartilage. OATS generally produces a roughened cartilage surface. ACI and MACI can generally produce results…[but] if repair can be initiated without surgery, we can save countless patients from severe complications, such as infection, blood clots, and the need for more surgery (4).
In our 2022 article How Can Regenerative Medicine Prevent Cartilage Loss?, we provide a detailed discussion of the nature and grades of cartilage degeneration. There is a discussion of how Platelet Rich Plasma (PRP) or Bone Marrow Concentrate (BMAC) is the best strategy to maintain what cartilage you have and decrease joint pain without the complications inherent to surgery.
Additionally, Chris Centeno, MD writes about a few cartilage defect cases he had success treating. The image below shows the pre and post MRIs of a knee that underwent a BMAC procedure. The MRI studies are one year apart (4):
This particular patient received a procedure at the Regenexx Cayman clinic with culture-expanded mesenchymal bone marrow cells. The culture-expanded bone marrow substance is then placed, or rather dripped like mortar or caulking, directly onto the lesion. The precision is achieved through image-guidance with a diagnostic ultrasound and live x-ray. This patient reported a decrease in pain, increase in function, and the image demonstrates a positive change in the cartilage defect and bone marrow edema a year after the procedure.
The Takeaway?
There are a handful of ways to repair cartilage. Some studies show a decrease in pain after 12 months with a MACI surgery (6), for example. However, our physicians’ empirical data from working with patients after such surgeries include a cascade of complications ranging from bone spurs to other areas of dead bone in the knee. Our stance always is to be as non-invasive as possible. At our Regenexx at New Regeneration Orthopedics of Florida clinics or Regenexx Cayman clinic, we offer proven and effective relief for injuries to cartilage of the joint. If this sounds like it could help you or someone you love, don’t hesitate to reach out today!
References:
- https://www.mayoclinic.org/medical-professionals/orthopedic-surgery/news/novel-stem-cell-therapy-for-repair-of-knee-cartilage/mac-20450891
- https://www.premierortho.org/services/knee/osteochondral-autologous-oats/
- https://healthjade.net/microfracture/
- https://regenexx.com/blog/possible-stem-cell-based-cartilage-regrowth/
- https://newregenortho.com/how-can-regenerative-medicine-help-my-cartilage-loss/
- https://pubmed.ncbi.nlm.nih.gov/25218576/