One of the most common reasons patients come into our clinics is due to a loss of cartilage in the knee. Phrases like “I have zero cartilage left,” “my knee is bone on bone,” or “I have severe knee arthritis.” There are all very common phrases we hear when patients come in with knee pain.
The other most common feature of these phrases is that at the root of it all, this pain is what is preventing them from doing what they love. The question is: How can regenerative medicine help?
Cartilage Deterioration is Prevalent in Knees
In a retrospective cohort study, the prevalence of severe cartilage damage was compared in the ankle and knee joints(1).
The study evaluated the degenerative change in cartilage, ranging from Grade 0 (intact cartilage with a healthy consistency) to Grade 4 (50% thickness of cartilage thickness defect and injury to the bone underneath the cartilage)- Table 1 defines each grade(1).

Figure 1 is a chart demonstrating the different cartilage changes from Grade 0 – Grade 4 and their prevalence in the knee versus the ankle.
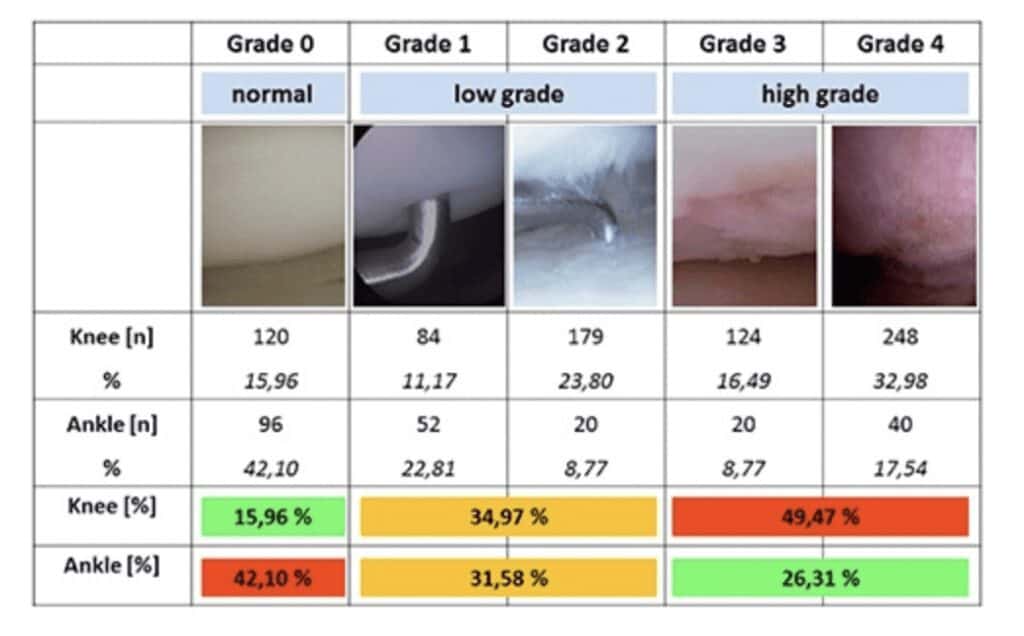
The study found “there is a higher prevalence of high-grade cartilage lesions (grade 3 and 4) in the knee (49.47%) compared to the ankle (26.31%)” (1).
What merits our attention from these findings is that the knee pain commonly involves a high grade of cartilage deterioration, but also involves an injury of the subchondral bone.
This is so important, it must be repeated – the most progressed grade of cartilage deterioration also includes damage to the subchondral bone, or the bone right underneath the damaged cartilage. What is causing the knee pain of these patients with advanced cartilage lesions?
What Is Causing Your Knee Pain?
The deteriorated cartilage is not what is causing your knee pain. It’s actually quite common for patients to have a very arthritic joint (eg bone-on-bone), with virtually no cartilage, and experience little to no pain.
This is possible because the cartilage actually is void of nerve endings, so there is no pain sensation in the cartilage itself. However, knee pain in the presence of arthritis is most definitely real and valid; so, what’s causing the pain?
When the cartilage surface has broken down, it compromises the strength of the bone. The bone, with the presence of healthy cartilage, is able to withstand the repetitive loads; however, when the cartilage is compromised, the bone experienced repetitive microtrauma.
The evidence of this shows up radiographically as inflammation deep to the bone and cartilage. The repetitive trauma unprotected by healthy cartilage shows up as visible bone marrow lesions (BML) on an MRI. This inflammation in the framework of the bone can be what is painful in an arthritic knee with cartilage damage.
How Can you Treat Knee Pain in the case of Cartilage Loss and BMLs?
There are a few procedures designed to “regrow” cartilage. All of the procedures to date are surgical, meaning they are more invasive than injection-based procedures. There has been a huge evolution in this technology. This evolution has come naturally as the long-term effects of certain surgeries can lead to some other issues down the line(5).
The original, most primitive version of cartilage repair microfracture (MF), is basically a surgery to make holes in the cartilage and bone so that bone marrow is released in order to promote healing in the area.
Then, other iterations have emerged like OATS, which uses grafts of a patient’s cartilage in one area is transferred to the “holes” in the damaged cartilage.
Autologous Chondrocyte Implantation (ACI) is a surgery where culture-grown cartilage cells are implanted into the damaged cartilage. In the most modern iteration, MACI or Matrix-Applied
Chondrocyte Implantation is a process where cartilage cells are taken from a patient, grown in a lab much like ACI. However, MACI takes it a step further because then these culture-expanded cartilage cells are loaded into a collagen matrix. The cells in the matrix are re-implanted into the same patient’s knee in an attempt to replace the damaged cartilage(4).
Chris Centeno, MD of the Centeno-Shultz Clinic states:
“I’ve seen countless patients through the years who have had each of these surgeries and I’ve never seen one produce a perfect cartilage repair. Microfracture often leaves dead bone behind or large bone spurs in the cartilage. OATS generally produces a roughened cartilage surface. ACI and MACI can generally produce results…[but] if repair can be initiated without surgery, we can save countless patients from severe complications, such as infection, blood clots, and the need for more surgery”(5).
So, what’s the solution then?
In our Regenexx clinics, we use bone marrow concentrate to treat knees with arthritis and cartilage loss or damage. Although it is not proven that the cells from the bone marrow concentrate can regenerate damaged or missing cartilage, it can be hugely effective in decreasing your pain.
There are four major ways that using regenerative medicine injections of bone marrow concentrate can reduce or eliminate pain in patients with joint arthritis and loss of cartilage:
- Cartilage: Improve and maintain the health of the existing cartilage to prevent further loss.
- Bone: Strengthen the matrix of the bone, especially where the bone has undergone the repetitive microtrauma from the loss of protective cartilage.
- Synovial Lining: The fluid within the joint itself is boosted by the growth factors to produce healthy chemicals instead of inflammatory, destructive ones.
- Ligaments/Tendons: Strengthen the ligaments and tendons for a more stable joint and better biomechanics.
Also, our physicians also promote healthful measures in addition to the procedures including bone marrow concentrate and/or PRP. It is important for the patient to work on making sure they address improving their biomechanics and adhering to the tenants of a lifestyle.
The key to getting the best outcome in a procedure in a knee with arthritis, unhealthy cartilage, and pain is to understand where the pain is coming from and create a well-rounded approach to treating it. Platelet Rich Plasma (PRP) and bone marrow concentrate (BMC) may be the best solution to decrease cartilage degeneration and pain associated with arthritis, but it is of the utmost importance to our physicians to look at the whole person.
Patients are able to get the best outcomes and influence their health when through attention to healthy eating, exercise, limiting chronic exposure to environmental toxicants/chemicals, better sleep, and use of certain supplements, more love and laughter, and having a sense of purpose (2). Additionally, it is important to identify the root cause of the issue and improving biomechanical imbalances that affect the joint.
So, while there are limited options for physically regrowing cartilage effectively and without surgery or complications, PRP oir BMC is the best strategy to maintain what cartilage you have and decrease joint pain.
References:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4274453/#:~:text=There%20is%20a%20higher%20prevalence%20of%20high%2Dgrade%20cartilage%20lesions,15.96%25%20of%20the%20knee%20joints.
- https://newregenortho.com/the-most-common-causes-of-cartilage-loss/
- https://regenexx.com/blog/ask-dr-c-episode-8-bone-on-bone-and-cartilage-regeneration/#gref
- https://www.ncbi.nlm.nih.gov/books/NBK424068/
- https://regenexx.com/blog/possible-stem-cell-based-cartilage-regrowth/#gref