The Rotator Cuff
The rotator cuff is a group of four muscles in the shoulder responsible for moving the ball of the shoulder through ranges of motions relative to the shoulder blade.
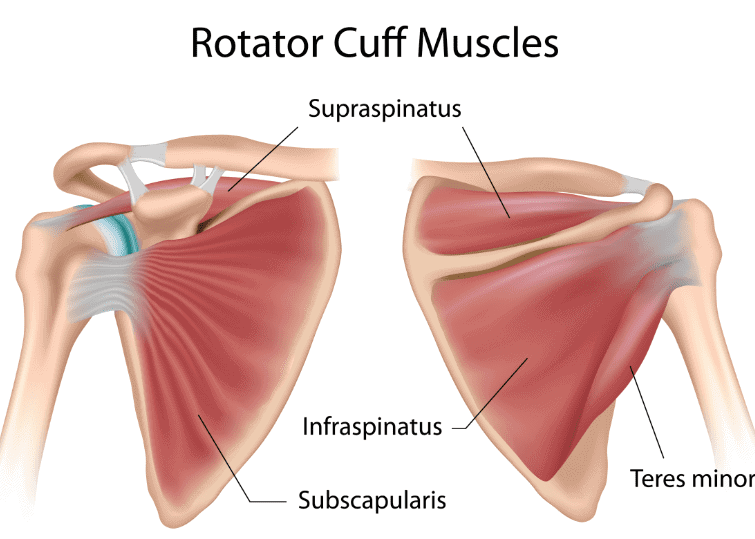
The muscles include:
- the supraspinatus which lifts the arm up overhead in abduction
- the infraspinatus which moves the shoulder in outward or external rotation
- the teres minor which moves the shoulder in outward of external rotation
- the subscapularis which moves the shoulder in inward or internal rotation
The rotator cuff is a vital system in the anatomy of the shoulder girdle; however, this joint’s breadth of range of motion puts stress and strain on them over the years. In fact, an epidemiological study found that the average rate of rotator cuff muscle tear is 22%, but the rate of tear increases in every decade of life, reaching up to 40% in the elderly population (1).
The tears can occur in any of the four muscles, but the Supraspinatus and Infraspinatus are the most common. Symptoms of rotator cuff tears are pain and weakness in range of motion of the shoulder and a generalized ache.
Traditional orthopedics has been surgically repairing rotator cuff repairs for decades, but it’s important to challenge the status quo to see if there is something better. Read on for research of the efficacy of rotator cuff repair surgery and the possibility of a non-surgical option.
Types of Rotator Cuff Tears
When discussing rotator cuff repairs, the extent of the tear matters when considering the prognosis of a surgery or procedure. Below are images of different grades of rotator cuff tears.

A partial-thickness rotator cuff tear is when a potion of the fibers are torn, but the majority of the tendon is still intact. A full thickness tear that is retracted is where the entirety of the tendon has torn and the two ends have snapped back, away from each other. The full thickness non-retracted tear is when at least a few fibers remain intact, causing the ends of the tendon to stay closely approximated. In his article on “Why You May Want to Avoid Rotator Cuff Repair Surgery,” Chris Centeno, MD observes full thickness non-retracted tears:
…constitutes about 1/2 of those patients that eventually get surgical repairs. Also, this naming convention is often missed on MRI reports, so a radiologist may spell this out differently. For example, the radiologist may write something like, “the supraspinatus tendon has high signal throughout more than 50% with intact fibers and minimal retraction.” (2)
The Challenge with Rotator Cuff Surgery
Usually rotator cuff repair surgery is recommended in traditional orthopedics when a patient fails to improve after six weeks in physical therapy. Even then, a battery of research exists evaluating the long-term efficacy of a rotator cuff tear repair surgery. One systematic review in particular analyzes the retear rate of rotator cuff repair surgeries. This study’s aim was to analyze existing studies to measure the retear rate after rotator cuff repair surgeries and evaluate the common reasons for retears. The systematic review included 31 articles, and retear rates averaged 21% at both 3-6 months and 12-24 months after surgery.
The systematic review also found the reasons for these retear rates were multifactorial, including both patient-related factors and non-patient-related factors. Examples of patient-related factors are fatty infiltration of the muscle or a large tear. Non-patient-related factors included post-op rehab protocols or surgical techniques.
With the retear rate of rotator cuff repair surgeries pushing one quarter of the surgical cases, the question can be raised: is there a better treatment option?
Research Supporting Regenerative Medicine for Rotator Cuff Repairs
Regenexx Tampa Bay at New Regeneration Orthopedics (NRO) is a trusted alternative to orthopedic surgery in Tampa, St. Petersburg, Sarasota, and Orlando, Florida. In the case of alternatives to rotator cuff repair surgery, NRO has been performing rotator cuff repairs with bone marrow concentrate into complete non-retracted rotator cuff tears for over a decade. In this procedure, a patient’s bone marrow is extracted from their pelvis and then the bone marrow is then processed in a state-of-the- art laboratory to release the mesenchymal cells and growth factors. The mesenchymal cells, or bone marrow concentrate (BMC), is then injected into the tear of the rotator cuff under ultrasound guidance. The ultrasound guidance is for precise placement of the BMC, which is paramount in this regenerative alternative to surgery.
Not only have physicians and patients across the entire Regenexx network appreciated the benefits of BMC in the rotator cuff, but Chris Centeno, MD et. al. are performing a randomized controlled trial (RCT) of BMC into rotator cuff tears. This RCT compares the result of the tears treated by BMC as compared to doing physical therapy alone. In the mid-term analysis paper for this RCT published in January of 2022, the BMC performed better than physical therapy (4).
The Takeaway?
Common approaches to complete non-retracted rotator cuff repairs in traditional orthopedic medicine are physical therapy or rotator cuff repair surgeries. Midterm data shows compelling evidence that a BMC procedure beats out physical therapy in patient pain and function scores. Further, a systematic review illustrated rotator cuff repair surgeries have up to a 21% retear recurrence rate.
If the conservative physical therapy option hasn’t been getting you back to doing what you love, the nonsurgical alternative could be a great option for you. Come see us to see if you are a candidate for the regenerative alternative for your shoulder pain.
References:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3768248/
- https://regenexx.com/blog/why-you-might-want-to-avoid-rotator-cuff-surgery/
- Longo, U.G., Carnevale, A., Piergentili, I. et al. Retear rates after rotator cuff surgery: a systematic review and meta-analysis. BMC Musculoskelet Disord 22, 749 (2021). https://doi.org/10.1186/s12891-021-04634-6
- Centeno C, Fausel Z, Stemper I, Azuike U, Dodson E. A Randomized Controlled Trial of the Treatment of Rotator Cuff Tears with Bone Marrow Concentrate and Platelet Products Compared to Exercise Therapy: A Midterm Analysis. Stem Cells Int. 2020 Jan 30;2020:5962354. doi: 10.1155/2020/5962354. PMID: 32399045; PMCID: PMC7204132.










