Acromioplasty is a surgical procedure of the shoulder also known as subacromial decompression surgery. Patients who have an acromioplasty commonly have the procedure done along with a rotator cuff repair.
During an acromioplasty, the surgeon shaves a spur that is usually on the undersurface of the acromioclavicular (AC) joint and the closely associated ligament structures.
The logic behind this is that the spur is theoretically impinging the rotator cuff, however, it has been shown that the spur itself does not cause impingement and that it usually significantly pre-dates the onset of symptoms.
So, removing the spur would, again theoretically, open up the space in the shoulder freeing it up for movement and a reduction of pain, it would seem.
But complications can arise when you cut shoulder ligaments that serve to stabilize the joint and research has not supported this surgery as being clinically more effective than non-surgical strategies.
Other issues can arise as a consequence of this surgery, including shoulder arthritis, more rotator cuff damage, and shoulder instability. Only a small percentage of patients with this condition would benefit from surgery and there are non-surgical ways to get better results.
The video (above) shows a live look at a moving x-ray of a patient’s shoulder instability as a result of an aggressive AC joint resection, which is a more comprehensive version of an acromioplasty.
In this post, we’ll dive deeper into the potential negative consequences that can happen after an acromioplasty.
About the AC Joint
Finding the AC joint on your own body should be fairly simple. Just put your fingers on the collarbone, or clavicle, next to your neck and run your fingers along the collarbone toward your shoulder.
The collarbone will feel smooth at first, and then you’ll come to a place where it rises to meet the shoulder’s top curve. This bump is the AC joint and right after it you’ll discover the acromion bone of the shoulder. The intersection of these two bones is what gives the acromioclavicular joint its name.
If this joint becomes arthritic or misshapen, a spur on the underside could possibly impinge on the rotator cuff. Physical therapy and/or a cortisone injection is often the first way that providers try to resolve the pain. Should these not help, many times, an acromioplasty surgery is offered as another option.
An invasive and permanent procedure, an acromioplasty shaves off parts of bones that are thought to be pressing on the rotator cuff and also may remove or destabilize supporting ligaments. There is scientific evidence that suggests this procedure rarely makes sense.
Acromioplasty Research
Unsurprisingly, multiple studies give acromioplasty a poor grade. One large, randomized controlled trial indicated that performing an acromioplasty along with a rotator cuff doesn’t have positive effects.
To quote the study, it said its findings were “consistent with previous research reports in which there was no difference in functional and quality-of-life indices for patients who had rotator cuff repair with or without acromioplasty.”
However, adding an acromioplasty does complicate the patient’s rehabilitation, making for a more challenging and lengthier recovery period.
Another study gave proof that surgery for rotator cuff tears caused by wear and tear – whether rotator cuff repair was done by itself or with acromioplasty – didn’t compete with physical therapy’s positive results.
Rotator cuff repair with acromioplasty is the U.S.’s most commonly performed shoulder procedure but it actually fails to accomplish its intended outcome. It’s meant to relieve the damaged rotator cuff from pressure but, in reality, the procedure makes it worse by making the structures less stable.
The authors of a study drew the conclusion that after an acromioplasty, the rotator cuff force needed to maintain normal glenohumeral joint biomechanics went up by 25 to 30%.
A Visual Depiction of Shoulder Surgery Complications from an AC Resection
When you watch the video at the beginning of this blog post, you will see a live, moving x-ray of a patient’s shoulder post-surgery. He underwent an AC joint resection, which created a large space between his collarbone and his shoulder. This gap will likely bring about further issues and make the shoulder unstable.
At the start of the video, the patient’s shoulder can be seen relaxed and down. The large gap is very visible. The gap narrows when he moves his shoulder up. This space was previously the AC joint, and also contained stability-creating ligaments.
Each time the patient moves his arm, his now unstable AC joint has excess movement. This particular patient reported worsening pain after his resection.
The visual evidence alone shows that removing parts the AC joint, a more extreme surgery than its related acromioplasty, causes additional issues, more than the procedure resolves.
Plus, studies repeatedly indicate that an acromioplasty doesn’t enhance a rotator cuff repair. It often makes it worse. Why, then, is an acromioplasty performed so often? It might work well for a small number of patients, but for most people, it should be avoided. After all, a biomechanical alteration like this is extreme and irreversible.
Since there are alternative options and a great number of risks associated with shoulder decompression surgery, you may want to just say no while you explore your options.
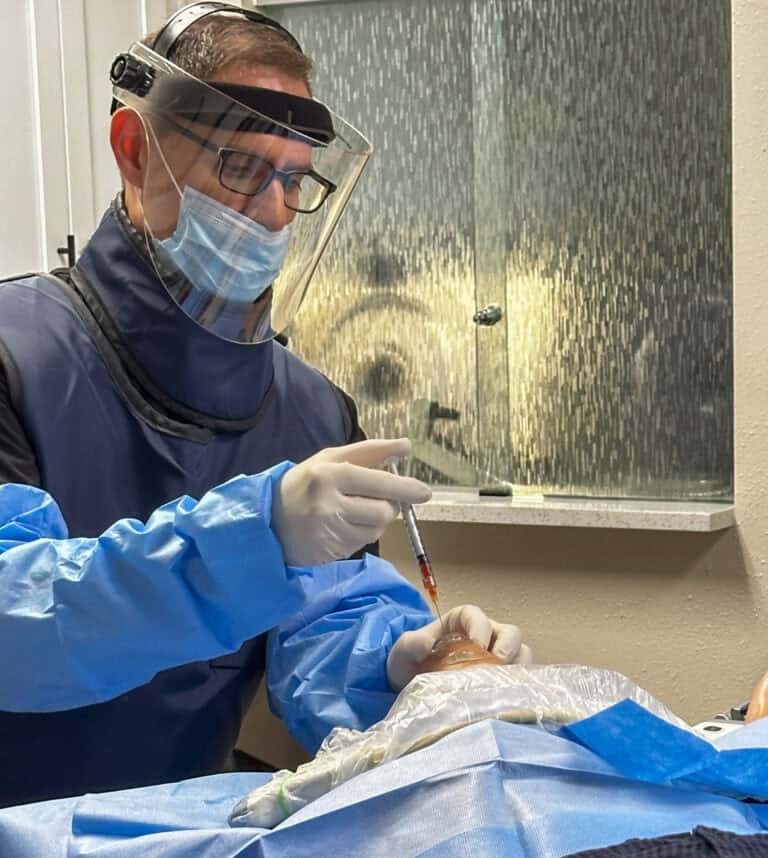
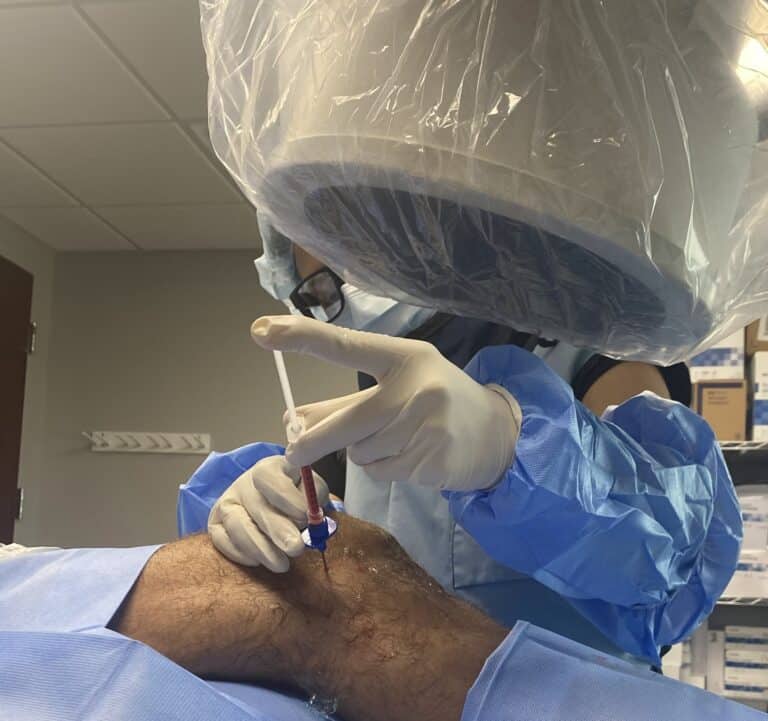
Regenexx procedures utilize one’s own concentrated platelets/growth factors and/or concentrated bone marrow to strengthen rotator cuff and ligament tissue and to change the microenvironment of the joints such that it favors healing and less inflammation.
A 2 year randomized controlled trial showed that a Regenexx procedure utilizing bone marrow for rotator cuff tears showed that patients reported a mean 89% improvement at 24 months, with sustained functional gains and pain reduction. MRI review showed a size decrease of most tears, regardless of whether a spur was present.
Our Regenexx Procedure Candidate Form is a great place to start understanding if regenerative orthopedic medicine is right for you.