In healthcare, there are a few variables at play that dictate what procedures patients seek and ultimately get. Of these variables, two of the most common questions that drive decisions are:
- What is the highest level of quality procedure that can give me long-term relief?
- What is the most cost-effective procedure?/ What will my insurance cover?
Unfortunately, there is a significant lag in the insurance-coverage landscape catching up with medical technology. This means that new, effective medical technology emerges but what insurance will cover can still be locked in the 1990s. Meanwhile, the cutting-edge in orthopedic procedures are still gaining research-powered evidence to support the safety and efficacy that will eventually get insurances on board to cover them.
Medical Technology & Insurance Coverage
In orthopedics specifically, it takes a lot of time for any new technology to be covered by insurance. There are steps that every procedure, substance, or device must pass through to gain FDA approval. FDA approval means “the agency has determined that the ‘benefits of the product outweigh the known risks for the intended use.’” However, the good news is the FDA does not “approve” or “not approve” medical procedures (like gall bladder surgery for example). Regenexx is considered a medical procedure. Regenexx is in compliance with all procedure codes; the FDA does not have any issues with the procedures we offer in the U.S. However, there are some bad actors out there who are egregiously out of compliance with regenerative procedure codes. More on that here.
Compliance is one thing, but the other side of FDA approval is that FDA approval often drives insurance coverage. For example, total knee replacements (TKR) are covered by insurance, but a treatment of Bone Marrow Concentrate (BMC) is not, even though there are compelling studies demonstrating that BMC-treated knees do better over time than their knee-replacement counterparts. One of the studies reviewed in this article spans 15 years, comparing BMC-treated knees and TKR-treated knees, and the 15-year pain level and function results were in favor of the BMC procedure.
So, since we now know that criterion number two (What will my insurance cover?) in our list does not always equal number one (What is the highest level of quality and efficacy when it comes to a procedure?) I wanted to discuss the spectrum of orthopedic procedures ranging from Regenerative to full-blown artificial/replacement and what these choices could mean for your body.
Remember the blog we recently posted on Evidence-Based Medicine? Well, this information will be hugely impactful in helping you to become an informed consumer of orthopedic medicine.
When it comes to orthopedic medicine, there is a range of procedures that may be offered for your condition. The main thing to remember is that, in orthopedics, usually patients come in because they have some combination of pain and/or dysfunction that is limiting their quality of life in some way. This could be: limiting their ability to sleep through the night due to pain, perform at a high level in a sport due to an injury, or simply be able to get up and down off the floor with their grandchildren without four days of soreness afterward.
Regardless of the personal patient goal, the clinical goal is relief, and longevity of the procedure’s impact. Below is a graphic illustrating the types of interventional procedures available to offer relief and improved function to patients with orthopedic issues.
This is a summary of Interventional Pain Management (IPM), and these procedures are described by Chris Centeno, MD, as:
IPM or Interventional Pain Management is a field where the doctor uses precise image-guided procedures that don’t involve open surgery that can help patients in chronic pain. These are percutaneous procedures, meaning they can generally be performed without a scalpel and “through the skin.”
IPM options are all preferred over surgery, but even the most invasive of this bunch can still be done in a way that’s been coined as “minimally invasive.” Let’s take a look at what each of these procedures entail and what makes them have a net-negative or net-positive impact on the body.
Regenerative
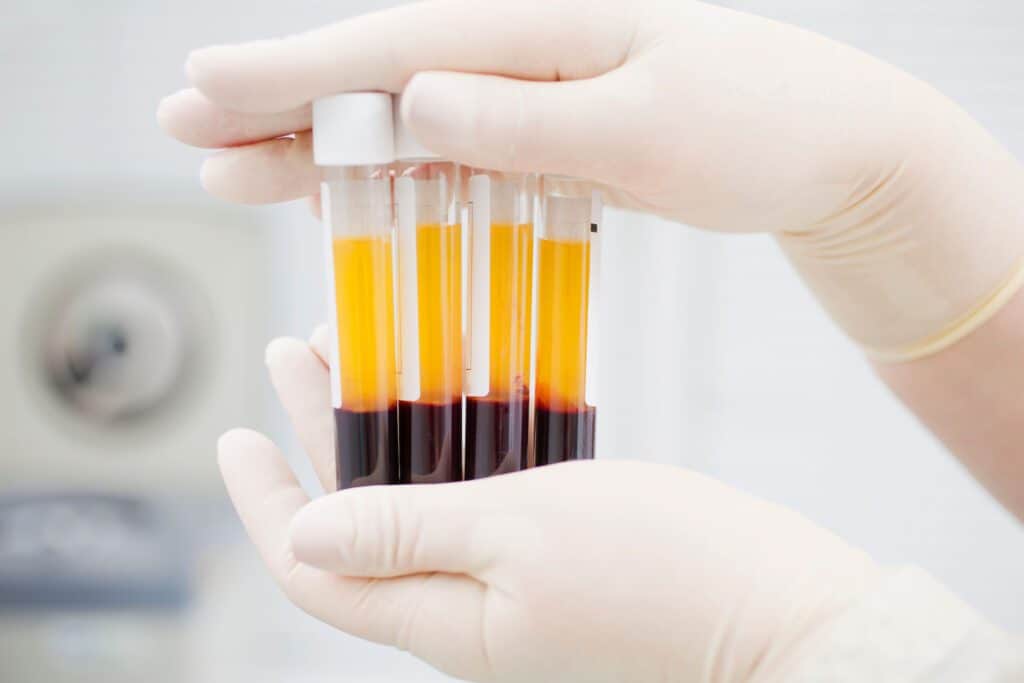
What is it? Regenerative medicine, what we specialize in here at Regenexx, is the type of medicine that has the ability to make damaged tissues like new. There is no other medical technology that is able to help a tissue strengthen and regenerate with its own substrate. This applies to tissue like tendons, ligaments, cartilage, nerves, and bone.
These procedures use PRP from the patient’s own blood or bone marrow concentrate to help any of the aforementioned tissues heal on their own.
Pro? Regenerative procedures are a net-positive procedure, meaning the impact improves the local tissues.
Con? Some patients find the out-of-pocket cost to be undesirable, because they are not always covered by insurance, and there are other orthopedic solutions that can be covered.
Progenerative
What is it? Chris Centeno, MD, coined this term to mean, “an orthobiologic that can help damaged tissue act more like normal, but that falls short of repairing it fully. So while not as good as growing new tissue to replace damaged tissue, it’s almost as good because it has no serious toxic side effects and it markedly increases function” (4). Conditions in this category include: more advanced joint arthritis, degenerative disc issues, radicular nerve pain, and severe tendon injuries or degeneration.
Pro? This is a net-positive option because they can improve conditions that are generally treated with surgery. These areas can then have less pain and more function as a result.
Con? Much like the regenerative category, some patients find the out-of-pocket cost to be undesirable when there are other orthopedic solutions that can be covered by insurance.
Anti-inflammatory (Non-Toxic)
What is it? Steroid injections are known to be harmful to surrounding tissues, which is why traditional doses of steroids will fall under our category of net-negative for tissue healing. Blocking inflammation for long-periods can be counterproductive in overall tissue regeneration goals. However, there are ways corticosteroids can be used in a net-positive therapeutic way. Most traditional corticosteroid injections are in doses that are milligrams, or 1,000,000x the naturally-occurring concentration in the body. So, when our physicians use corticosteroids, they use nanograms, which is a super tiny concentration that has anti-inflammatory effects without damaging surrounding tissues.
Pro? Decreases acute inflammation and swelling for quick relief, without damaging the whole person or the surrounding tissues.
Con? Relief is tricky. Of course we want to make our patients feel 100%, but “quick relief” is a tool to be used in specific situations, like an exorbitant amount of swelling, or acute pain that cannot get under control. But, this is a tool for those things and not the go-to. In regenerative medicine, our goal is to help the tissue regenerate, and although this is a pain-relief tool it does not regenerate tissue.
Anti-inflammatory (Toxic)
What is it? This is the traditional corticosteroid that is very commonly used in orthopedics. It is a large-milligram dose that is one million times the normal amount of steroid the body uses on it’s own.
Pro? Quick relief, and these are often covered by insurance.
Con? These injections are so potent that they shut down natural biological processes that are able to help the body heal itself. It may mask pain, but it is a net-negative since it can have lasting effects on the adrenals, blood sugar control, and tissues.
Percutaneous-Surgical
What is it? Percutaneous surgical is a fancy term for “scope.” You hear the Phrase, “I got my knee scoped” or “they needed to clean things up in my joint with a scope.” This is less invasive than a full-blown surgery because it scraps the scalpel and gets the job done with a smaller tool, but the problem is that the point of this is to remove parts and tissue. The body doesn’t have spare parts, so if something, like a part of a meniscus in the knee, is “snipped” or cleaned up during a scope, it changes the whole structural unit.
Pro? This is preferred over, and less invasive than, open surgery.
Con? Pathological parts, or pieces of anatomy, like a problematic knee meniscus, shoulder labrum, herniated disc, or carpal tunnel ligament, may cause issues as-is, and causing a snip/cut change, even through a scope, changes the bio-mechanics of that area forever. Areas that are treated via “removal of the broken part” are more susceptible to new issues down the line.
Ablative
What is it? Abation is a fancy word for “destroy.” The procedure that is ablative is called a Radiofrequency Ablation (RFA) and is used to decrease or eliminate the pain signals from nerves.
Pro? This procedure can eliminate nerve pain.
Con? The nerves that are killed off to reduce pain also carry functional signals. So, unfortunately there is no way to only affect the pain-producing nerves. The nerves that supply to stabilizing muscles of the area are also killed off. So, that means that with the pain reduction, function also takes a hit, which can lead to further dysfunction. Also, it is not uncommon for the pain nerves to regenerate over time, growing back stronger, with stronger pain signals.
Implant
What is it? Implants are foreign objects that are inserted in the body. For our discussion here, it includes things like SI Joint fusions for sacral pain, Interspinous spacers for arthritis in the facet joints, or even pain-relief simulators to block pain signals in low backs. All of these are various degrees of horrifying because they influence the body in hyper-unnatural ways that have evidence of failing and/or needing revision. These implants are invasive enough to open the Pandora’s box of orthopedic procedures. So, none of these solutions can beat the net-positive effect of regenerative procedures, which are options for these same pain complaints.
Pro? These seem to be solutions for those who feel like “they have exhausted all options,” and from a health psychology standpoint, there is a certain mystique around surgical and invasive procedures. Some patients feel their conditions to be “so broken” that these are their only options. These points are hardly a pro, but if I am reaching for some rationale here, it is because it can apply in these situations.
Con? These are foreign devices that have a net-negative impact on the body. One example is: SI Joint fusions limit movement in a joint that vitally depends on motion. As stated by Chris Centeno, MD, “in the long run, my experience to date shows that these systems don’t last and often need to be removed or revised.”

The Takeaway
Every level of interventional pain management discussed here has a pro/con list as it comes to efficacy versus invasiveness versus net positive/negative to the body versus out-of-pocket cost. The goal here is to inform you, as a consumer, of what the physical drawbacks are if you’re trying to maximize insurance and reduce your out-of-pocket cost. This list is intended to give you a clear idea of which route would give your injury and function the most relief, with the most longevity.
We feel that it is logical to choose from the three net-positive options on our list, given the opportunity, but our medical system is insurance-centric, which would eliminate those out of the gate. It is the job of good clinicians to tell patients the full spectrum of the risks, benefits and alternatives to the procedures they might choose for their conditions.
Since cost is such an emotionally-charged subject when it comes to healthcare, it is something the Regenexx Provider Network takes very seriously. Since approaching global insurance coverage through traditional methods like FDA approvals and clinical trials takes time, Regenexx is able to go directly to companies with self-funded insurance.
A company with self-funded insurance has their own money allocated to spend on all of their employees’ healthcare expenses. So, it makes sense that the company wants to make sure every healthcare dollar is spent wisely and their employees can get the most benefit for the least amount of money, and not to mention time out of the office. Usually in these companies, they will track episodic claims, meaning that if someone has back pain that ebbs and flows over two years, the total amount spent on that pain for two years of therapy, MRIs, and steroid injections are totaled. So, if one regenerative procedure can be less than the two years of ongoing expenses, many companies opt to go with Regenexx as their in-house orthopedic recommendation. The most exciting thing about a company making REgenexx an added benefit, is that they will pay for their employee’s treatment because they know it saves time and money in the long run.
The takeaway? Make sure you do your homework, not only to cost-compare, but to know what a proposed orthopedic procedure may do to your body in a net-positive or a net-negative way. Our Regenexx at New Regeneration Orthopedics physicians would love to talk through the best options for your orthopedic condition.